Medical flight transport cost usually falls between $12,000 and $80,000. In many cases, a relatively short trip can still be expensive, and a 100-mile transport can exceed $40,000 before extra medical staffing or international logistics are added.
If you're reading this while trying to move a parent, spouse, child, or patient, you're probably dealing with two pressures at once. One is medical urgency. The other is financial uncertainty. Families want to know one thing fast: what will this cost, what will insurance pay, and how do we avoid making a bad decision under stress?
Those are the right questions. The problem is that most articles stop at a price range and never explain what drives the bill, why one flight quote looks nothing like another, or why insured patients still end up with major balances. A useful answer has to cover both medicine and logistics, because air transport sits right at the intersection of the two.
Understanding Medical Flights and Their Purpose
A medical flight isn't just a private plane with a stretcher. It's a coordinated medical transfer built around a patient who can't safely travel by standard means, or who can't afford the time a ground route would take.
In practical terms, a medical flight is used when three things come together:
- The patient needs monitored care in transit. That might mean oxygen, cardiac monitoring, medication management, airway support, or ICU-level observation.
- The distance changes the risk. A patient who might tolerate a short local ambulance ride may not tolerate hours on the road.
- Time matters clinically. Trauma, stroke recovery transfers, cardiac cases, neonatal and pediatric transfers, and complex post-surgical moves can all depend on reaching the next facility quickly.
For many families, the first confusion is whether they are dealing with an emergency helicopter response or a planned hospital-to-hospital transfer. Those are very different situations.
Emergency and non-emergency flights
An emergency flight usually starts at the scene or at a facility that can't provide the next level of care fast enough. Helicopters often fill that role because they can cut response time across difficult terrain or long rural distances.
A non-emergency medical flight is often a fixed-wing aircraft arranged from one hospital to another, from a rehab center to a specialty hospital, or from an out-of-state facility back closer to home. Non-emergency doesn't mean unnecessary. It usually means the transport is urgent enough to require air, but organized with more planning.
A medical flight becomes necessary when the patient's condition, route, and timing all point to the same conclusion: ordinary travel isn't safe enough.
What families usually need to decide first
Before anyone talks aircraft, a coordinator has to answer a more basic question. Is air the right mode?
That decision normally depends on:
- Current clinical status. Stable, fragile, or actively critical.
- Transport tolerance. Can the patient sit up, lie flat, handle cabin altitude, or withstand a long drive?
- Destination requirements. Is the receiving hospital expecting immediate arrival for a bed, specialist, or procedure?
- Transfer window. Some patients need same-day movement. Others can wait for a more cost-conscious option.
If you want a plain-language explanation of what an air ambulance team handles from bedside to bedside, this overview of what an air ambulance really does is helpful.
Decoding the Medical Flight Transport Cost Breakdown
The fastest way to understand medical flight transport cost can be broken down into three layers. First, there's the aircraft launch cost. Second, there's the distance cost. Third, there are the clinical and logistical services wrapped around the flight.
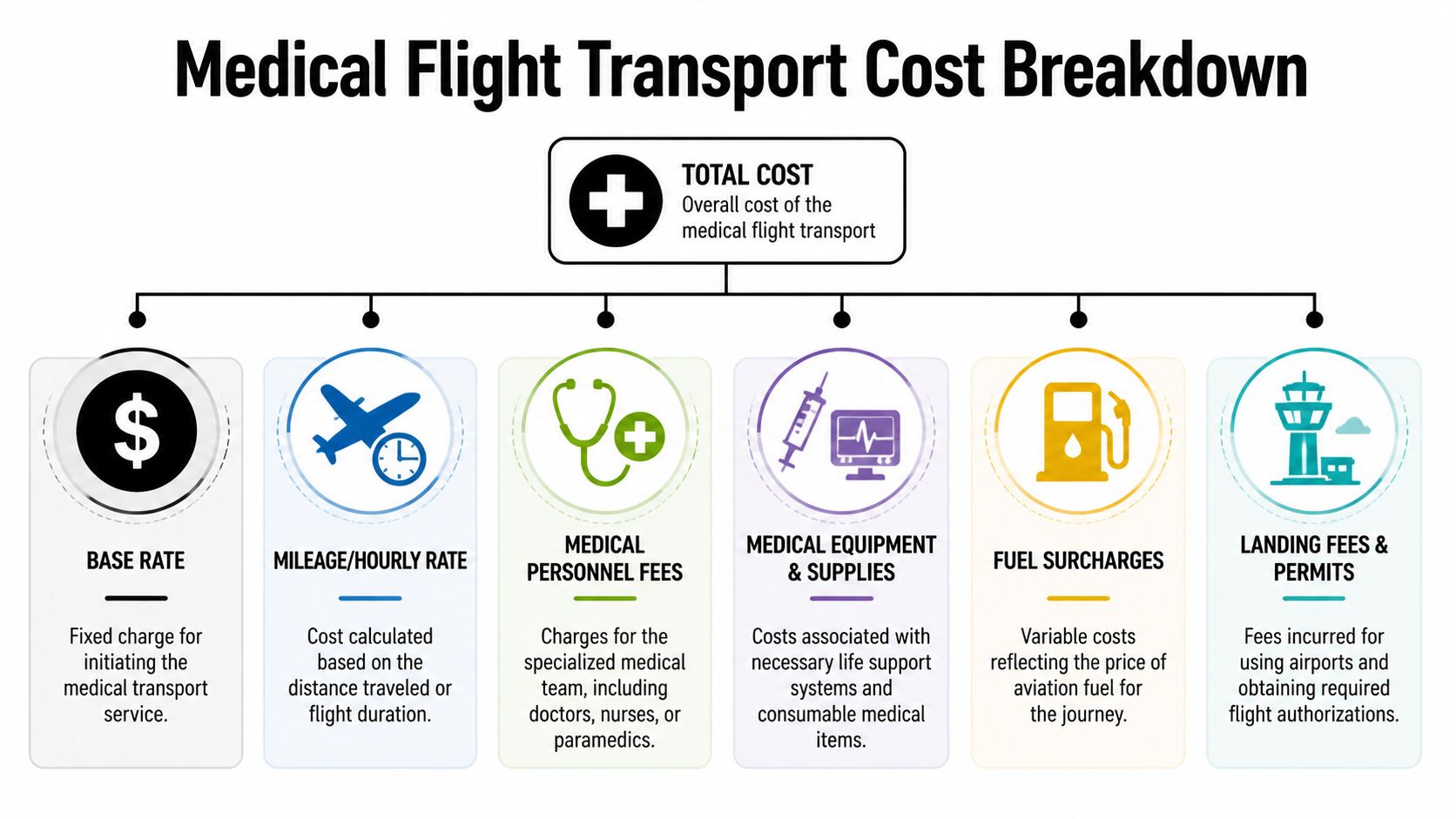
The two charges that shape the bill
Air ambulance pricing commonly starts with a liftoff or base fee plus a per-mile charge. Reported liftoff fees range from $8,500 to $15,200, and per-mile charges range from $26 to $133 according to this air medical transport cost breakdown.
That same source explains why aircraft choice matters so much. Mileage represents 35% of total helicopter costs but 68% of fixed-wing plane costs, which means the same route can price differently depending on whether the mission uses a helicopter or a plane.
That structure is why short flights can still carry a large bill. The base fee doesn't disappear just because the route is modest.
Why the aircraft changes the economics
Helicopters and fixed-wing aircraft solve different problems.
Helicopters are built for direct access and short-response missions. They often handle scene pickups, roof helipads, and places where an airport transfer would add delay. Because of that, the fixed launch cost can loom large.
Fixed-wing aircraft are often the better fit for longer hospital-to-hospital movements. Mileage makes up more of their total cost, so distance affects the final bill more heavily. On the right route, they can also be the more practical medical platform.
Practical rule: Don't ask which aircraft is cheaper in general. Ask which aircraft is medically appropriate for this specific patient and route.
What else gets added to the quote
Families are often surprised that the aircraft is only part of the invoice. Common cost drivers include crew and equipment choices, airport logistics, and the ground segments before takeoff and after landing.
| Cost Component | Description | Impact on Total Cost |
|---|---|---|
| Base fee | Launch or liftoff charge for activating the aircraft and crew | High on short routes |
| Mileage | Per-mile flight charge | Increases with distance, especially for fixed-wing |
| Medical personnel | Nurse, paramedic, respiratory support, or other required clinicians | Rises with patient acuity |
| Equipment and supplies | Ventilator, monitors, oxygen, infusion support, bariatric gear | Can materially increase total cost |
| Ground coordination | Ambulance to airport and from airport to facility | Adds bedside-to-bedside expense |
| Permits and airport handling | Operational and access-related charges | More visible on complex routes |
What works and what doesn't when reviewing quotes
What works is asking for a complete bedside-to-bedside quote. That means aircraft, medical crew, equipment, and both ground legs are spelled out.
What doesn't work is comparing two quotes that define the service differently. One company may include ground ambulances and ICU gear. Another may quote only the air segment, which makes the number look lower until later charges appear.
If you want a more aircraft-specific view of pricing variables, this medical plane cost guide gives useful context.
How Insurance Covers Air Ambulance Services
Insurance is usually the most stressful part of the conversation, and for good reason. Families hear "medically necessary" and assume that means "covered." It doesn't always work that way.
Why covered patients still get large bills
The biggest risk is network status. According to this analysis of private jet vs public medevac billing issues, 50% to 69% of medical flights are out-of-network, 72% of airlifted patients receive unexpected bills, and median charges are $36,400 for helicopters and $40,600 for jets.
That tells you something important. Even if the transport is appropriate, the payment path may still be messy.
In practice, a family can get approval language from an insurer and still face a dispute later over provider status, medical necessity wording, aircraft type, route, or documentation from the sending facility.
The questions to ask before the flight
When a case manager or family member calls insurance, broad questions don't help much. Ask specific ones and write down the answers.
- Air ambulance benefit. Does the plan cover helicopter, fixed-wing, or both?
- Medical necessity standard. What documentation does the insurer require from the physician?
- Authorization process. Is pre-authorization required, and if so, who must request it?
- Network status. Is the proposed transport company in-network or out-of-network?
- Ground segments. Are the ambulance transfers to and from the airport covered separately?
If an insurer says "it depends," ask what documents, codes, and physician notes they need to make the decision.
A good starting point for older adults and families working through federal coverage questions is this guide on whether Medicare covers air ambulance.
Documentation matters more than people expect
A denial often starts with paperwork gaps, not only with the clinical facts. The strongest file usually includes the physician order, current vitals and nursing notes, diagnosis summary, reason ground transport isn't appropriate, receiving facility acceptance, and a detailed transport quote.
This video offers a useful overview before you call the payer or coordinator:
What helps during claims and appeals
If coverage is uncertain, don't wait until after transport to organize records. Keep a timeline of every call, every name, and every reference number. Ask for email confirmation whenever possible.
A simple appeals file should contain:
- The medical reason air was required
- A statement explaining why ground was not clinically appropriate
- The sending and receiving physician documentation
- The itemized invoice and transport notes
- Any prior authorization or verbal approval records
Families who stay organized usually have a clearer path, even when the answer isn't immediate.
Actionable Steps to Manage and Reduce Expenses
Individuals cannot control whether a loved one needs air transport. They can control how the purchase is structured.
The biggest mistake is shopping by headline price. The smarter move is to compare scope, because missing services are often what turn a manageable quote into a painful final bill.
Ask for itemization, especially for complex cases
One persistent problem in this industry is the lack of transparent pricing for specialized transports. As noted in this long-distance medical transport guide, case managers arranging bariatric or ICU-level transfers can run into major unbudgeted overruns if quotes don't separately spell out extra equipment or staffing.
That matters because "medical flight" can mean very different things depending on the patient. A stable patient on oxygen is not the same mission as a ventilated ICU patient or a bariatric patient needing specialized loading, stretcher configuration, or additional crew support.
The questions that save money
These are the questions worth asking every provider:
- What's included from bedside to bedside. Confirm both ground legs, not just the flight.
- What clinical staffing is included. Ask whether the quote assumes a nurse-led crew, higher-acuity team, or added respiratory support.
- Are there specialized equipment charges. Bariatric gear, ICU monitoring, and other needs should appear in writing.
- What triggers a revised quote. Changes in patient condition can change staffing and aircraft requirements.
- What is the cancellation policy. Weather, physician hold, or a sudden decline in patient stability can alter the mission.
A low quote with vague language usually costs more than a higher quote with precise inclusions.
Options worth discussing
Not every case needs a dedicated air ambulance. For stable patients, a medical escort on a commercial itinerary or a long-distance ground option may be more realistic financially.
Some coordinators also ask about repositioning opportunities or other routing efficiencies when time allows. Availability is case-specific, but it can be worth the conversation.
If you're comparing providers, include one that offers a full coordination model. For example, Med Jets by Air Trek arranges air transport, medical escorts, and ground components as part of end-to-end patient transfer planning. That's one service model among several, but the value of any provider is in whether the quote matches the medical reality of the case.
Comparing Alternatives to Dedicated Medical Flights
A dedicated medical flight is not always the right answer. Sometimes it's the only safe answer. The difference comes down to patient stability, distance, and how much care must happen during transit.
Side-by-side practical comparison
| Option | Best fit | Medical capability | Speed | Comfort and control |
|---|---|---|---|---|
| Dedicated medical flight | Unstable, fragile, or ICU-level patients | Highest | Fastest over long distance | High control over care environment |
| Commercial flight with medical escort | Stable patients who can tolerate routine air travel | Moderate | Moderate | Less flexible, depends on airline rules |
| Long-distance ground ambulance | Patients who need monitoring but can tolerate road travel | Moderate to high depending on crew | Slower | Can work well for shorter regional moves |
| Personal vehicle | Very stable patients only | Minimal | Variable | Least suitable for medically complex travel |
When air can be the better value
People often assume air is automatically the least cost-effective option. That's too simple. A 1991 study on helicopter versus ground response economics found a helicopter service cost $2,811 per patient compared with $4,475 per patient for an equivalent ground network in that modeled setting, showing that rapid air response over a large service area can be more cost-effective in the right circumstances.
The old study doesn't tell you today's quote. It does explain something families see every day: sticker price and value are not the same thing.
What usually works best by scenario
- Dedicated flight works when the patient needs continuous advanced monitoring, fast transfer, or controlled loading and unloading.
- Commercial escort works when the patient is medically stable, can follow a scheduled route, and doesn't need an ICU-style environment.
- Ground ambulance works when road time is acceptable and the patient's condition allows a longer transport window.
The wrong choice is usually the one that tries to save money by underestimating the patient's needs.
Your Checklist for Arranging Medical Transport
When families are under pressure, checklists help. They keep important details from slipping through the cracks.
Use this order
Confirm the medical need
Ask the sending physician what level of monitoring, oxygen, medication support, and transport urgency the patient requires.Secure acceptance from the receiving facility
Make sure the destination hospital, rehab center, or specialty unit has accepted the patient and has a bed plan.Gather the core records
Collect the diagnosis summary, current medication list, recent vitals, nursing notes, imaging reports if relevant, and the physician transport order.Call insurance before authorizing transport
Ask the specific benefit and network questions covered earlier. Write down names, dates, and reference numbers.Request detailed quotes from more than one provider
Compare scope, not just the total.Verify bedside logistics
Confirm ground ambulances, pickup timing, who handles paperwork, and whether a family member may accompany the patient.Double-check patient-specific needs
Mention bariatric requirements, infection precautions, oxygen dependence, ventilator use, mobility limitations, and language needs upfront.
Clear information early usually leads to a safer transfer and a cleaner invoice later.
- Get the final written itinerary and inclusions
Before anyone moves the patient, make sure the family, case manager, and receiving team all have the same plan.
Common Questions About Medical Flight Costs
What do international medical flights usually cost
International transports usually land on the high end of the cost spectrum because routing, permits, customs coordination, airport handling, and medical staffing all get more complicated. General air ambulance pricing ranges from $12,000 to $80,000, and a 100-mile trip can exceed $40,000 even before international clearances or specialized medical teams are added, according to this air ambulance cost overview.
Can a family member travel with the patient
Often yes, but it depends on aircraft configuration, patient acuity, and weight-and-balance limits. Ask this at the quoting stage, not after the flight is scheduled. If a companion is important for communication or emotional support, say so early.
What about bariatric or ICU-level patients
Expect more planning. These transports may require specialized loading, additional equipment, or a higher-acuity medical team. The right next step is to request an itemized quote that clearly names every added clinical or equipment requirement.
What happens if the flight is delayed or canceled
Weather, airport restrictions, and changes in the patient's condition can all delay departure. Ask the provider how medical reassessment is handled, whether the crew can stand by, and what costs apply if the patient becomes temporarily unfit to fly.
How should I send records quickly and securely
Use a process built for healthcare paperwork, not a casual email thread. If you need a simple method for secure medical document submission, that kind of workflow can help families and case managers move records faster while keeping the file organized.
A medical flight bill can be intimidating, but the process becomes much more manageable when you break it into parts. First confirm the medical need. Then verify insurance. Then compare detailed, itemized logistics. In stressful situations, clarity is what protects both the patient and the family.

